Wet Macular Degeneration
What is wet age-related macular degeneration?
Age-related macular degeneration (AMD) is a breakdown of the macula in the eye. The macula is the center part of the retina, the light-sensitive tissue that lines the back of the eye. The macula is the part of the retina that we use for our most detailed vision work, like reading. When someone gets the wet form of AMD, abnormal blood vessels grow underneath the macula. These abnormal blood vessels are called choroidal neovascular (CNV) membranes and can produce tissue swelling, hemorrhage, and scarring. Although the damage to the macula can lead to loss of central vision, peripheral vision is normally preserved.
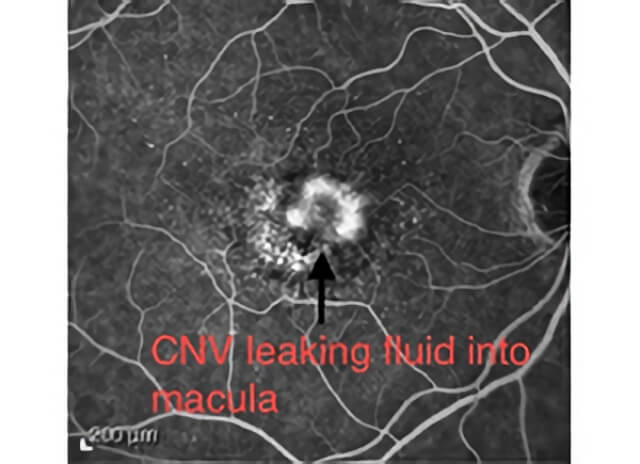
A fluorescein angiogram showing areas of abnormal leakage from choroidal neovascular membranes into the macula.
Learn more about wet age-related macular degeneration (AMD) at ASRS
Información en español en el sitio web de ASRS
Who is at risk for AMD?
AMD has many risk factors, including age over 50 years, a family history of AMD, and smoking. Caucasians1, especially those with lighter color and blue eyes are at higher risk
What causes wet AMD?
With aging, the layer under the retina thickens and the nutrient supply to the retina is disturbed. In response, Vascular Endothelial Growth Factor (VEGF) is released and abnormally high VEGF causes leaky blood vessels to grow under the retina. When these leaky vessels bleed, scarring and damage occur to the retina.
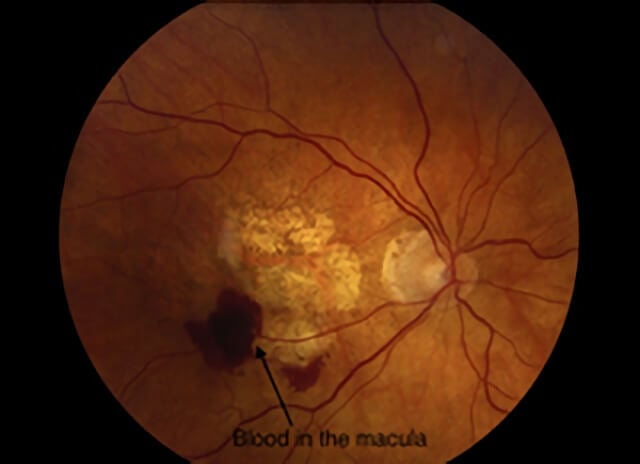
A color photograph showing bleeding in the macula from wet AMD.
How is wet AMD diagnosed?
Many times people first realize that they have a macular problem like wet AMD when they notice blurring, distorted lines, or missing spots in the vision. Examination of the retina with specialized lights and lenses after dilation of the pupils can discover signs of AMD. Computerized photographic tests such as a fluorescein angiogram (FA) and optical coherence tomography (OCT) help in evaluating the extent of damage and response to treatment. An FA is done by injecting an orange dye into a vein in the arm and taking special digital photographs of the dye as it flows through the blood vessels in the retina to look for abnormalities. An OCT is a painless computerized scan of the retina that provides a detailed view of the inner retinal structures.
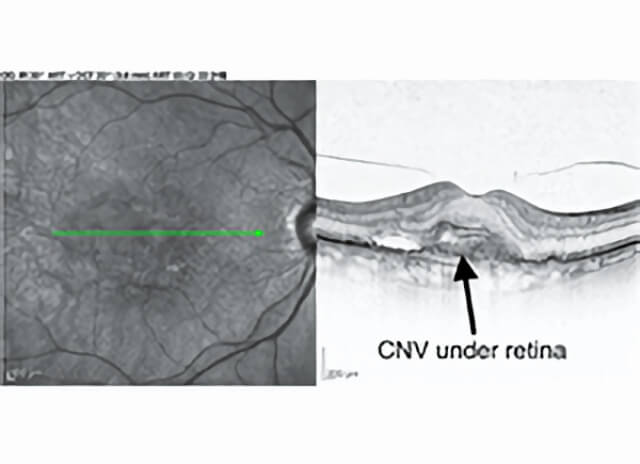
An OCT retina scan can show abnormal blood vessels (CNV) under the macula in wet AMD.
What can be done for Wet AMD?
How frequently do I need Injections?
The Anti-VEGF agents currently available last for 4-6 weeks before their effects fade and a new injection is typically needed. Most clinical trials show that treatment every 4-8 weeks gives the best results. Some patients need more frequent injections and others need less frequent injections. The intervals required by any one patient may change with time. Your doctor will decide with you how frequently you need treatment.
Does the injection hurt?
The procedure is quick and practically pain free for most patients. A sterile lid speculum helps keep the eye open and an antiseptic kills any germs. It is common for the eye to feel irritated and scratchy for a day after the injection. Worsening vision and severe pain, especially if it is not improving after the first day may be signs of an infection after an eye injection and if you have these symptoms you must contact your doctor.
Will I go blind from wet AMD?
With treatment and close follow up, today’s treatments for wet AMD can often preserve good vision for years. Even with the best treatment, it is possible that AMD may progress and lead to significant vision loss. If only one eye is affected by wet AMD, it is possible that they other eye may develop wet AMD at a later time. It is important to monitor both eyes and to follow your doctor’s instructions to maximize your chances of keeping your retinas as healthy as possible3. Although in severe cases, patients may lose their center vision from AMD and become unable to read or recognize faces easily, it is very rare for patients to become totally blind or to lose the ability to walk from AMD. Tools, magnifiers, and techniques, called low vision aids, can help many patients with vision affected by AMD lead a more normal life.
References
- Chang MA, Bressler SB, Munoz B, West SK. Racial differences and other risk factors for incidence and progression of age-related macular degeneration: Salisbury Eye Evaluation (SEE) Project. Invest Ophthalmol Vis Sci. 2008 Jun;49(6):2395-402. pubmed.ncbi.nlm.nih.gov/18263809
- Brown D, Heier JS, Boyer DS, Freund KB, Kaiser P, Kim JE, Sarraf D. Current Best Clinical Practices—Management of Neovascular AMD. Journal of VitreoRetinal Diseases. 2017; 1(5):294-297. journals.sagepub.com/doi/abs/10.1177/2474126417725946
- Ho AC, Albini TA, Brown DM, Boyer DS, Regillo CD, Heier JS. The Potential Importance of Detection of Neovascular Age-Related Macular Degeneration When Visual Acuity Is Relatively Good. JAMA Ophthalmol. 2017 Mar 1;135(3):268-273. pubmed.ncbi.nlm.nih.gov/28114653
Schedule Wet Macular Degeneration Treatment in Northern California with Retinal Consultants Medical Group
Since 1975, Retinal Consultants Medical Group has been providing outstanding care to patients throughout Northern California, including Sacramento, Modesto, and Stockton. Our retina specialists and surgeons treat multiple vitreoretinal conditions, such as age-related macular degeneration and diabetic retinopathy. We invite you to contact us with any questions or schedule an appointment today.


