Pars Planitis
What is pars planitis?
The term uveitis refers broadly to a group of rare disorders in which the white blood cells of the immune system flood into the interior of the eye leading to uncontrolled inflammation. Pars planitis is is a form of uveitis that can affect persons of any age, race or gender. In this disorder, inflammation is concentrated within the eye’s midsection, called the pars plana. Over time, the accumulation of white cells damages the lens and iris as well as the retina. Although it is unusual for patients to become blind from pars planitis as many as 20% can suffer visual loss if the condition goes untreated.
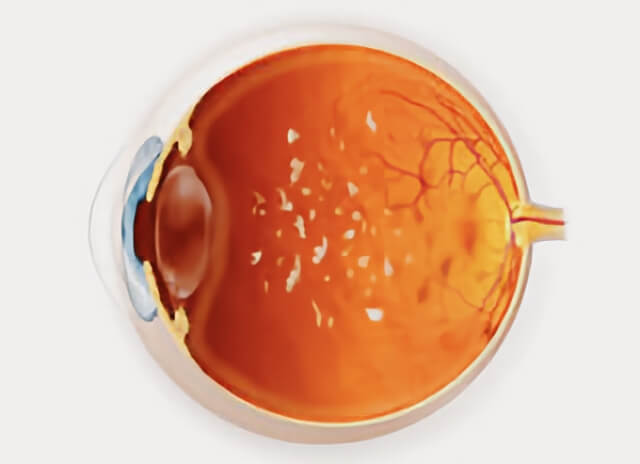
In pars planitis, a form of uveitis, inflammatory debris forms in the vitreous cavity located in the interior of the eye. This debris can block the vision or be seen by the patient as “floaters.”
Learn more about Pars Planitis
What are the symptoms of pars planitis?
Once the pars plana develops inflammation, large clusters of cells and debris disperse into to the center of the eye and lodge in the vitreous, normally a crystal clear jelly-like substance that occupies the central cavity of the globe. These opaque clumps cast shadows onto the retina and are perceived as “junk” floating in the visual field. This debris is readily visible to your ophthalmologist during your examination. The medical term for this is “vitritis” and its effects can reach the lens and iris, leading to cataract and scarring, and to the central retina, leading to swelling of the macula and blurred vision. The swelling of the retina caused by pars planitis is known as cystoid macular edema.
In many cases, the inflammatory debris is minimal and gravity tends to pulls it to the bottom of the eye where it cannot impede vision. Sometimes, the inflammation can be so severe as to permanently affect the ability of the eye to see. This is because the fluids in the front of the eye are constantly recycling, unlike the static, gel-like quality of the vitreous. Depending on the amount and density of material that infiltrates the vitreous, the length of time it takes for vision to improve is highly variable. On occasion, surgery is indicated to clear severely clouded vitreous.
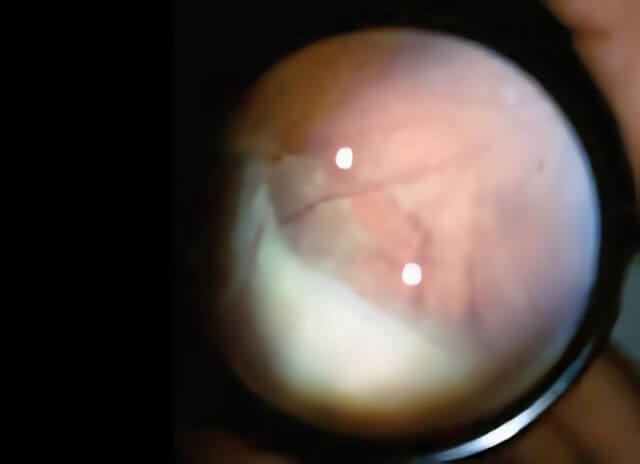
In this photograph, the inflammatory debris from pars planitis is visible as a “snowbank” on the retina in the lower left portion of the image.
What causes pars planitis?
Although the cause remains unknown, it is believed to be an autoimmune disease analogous to rheumatoid arthritis, in which the immune system inappropriately begins to attack the body, in this case the center of the eye. In the majority of cases, the cause of pars planitis is unknown, termed “idiopathic” in medical parlance, and is unrelated to any other disease of the body about 70% of the time. In about 30% of cases, pars planitis is associated with another disease, such as sarcoidosis (22%), multiple sclerosis (8%), and Lyme disease (less that 1 percent). Your doctor will order certain tests to look for these rare but important associated diseases.
How does pars planitis affect the eye?
The damage caused by chronic inflammation is insidious. Superficially, the eye appears white and healthy, but inside the white cells that normally fight infection injure important ocular structures critical for good vision. For example, a common complication is the development of a cataract as the natural lens loses its clarity. The pupil, which normally glides smoothly over the lens, can become contracted and scarred. Chronic inflammation eventually damages the drainage outflow of the eye, leading to elevated intraocular pressure and the onset of severe inflammatory glaucoma. The retina located in the lower perimeter of the globe can atrophy and bleed into the vitreous. The central macula can become overloaded with fluid, permanently reducing the ability of the eye to see fine detail. Early diagnosis of pars planitis is important because once vision loss has occurred it is very difficult to reverse. The disease is characterized by periodic exacerbations and remissions over many years so it is vital that patients undergo careful eye exams from an expert in the field of uveitis and vitreoretinal diseases. Treatment must be tailored to an individual’s specific needs in an effort to prevent vision loss or to intervene when necessary to correct problems as they arise.
How is pars planitis treated?
Pars planitis is not curable, but it is a treatable condition. Sight preserving therapy may include the use of injectable or oral medication, and/or surgery to halt disease progression.
We do not recommend the chronic use of steroid eye drops to treat pars planitis because they cannot penetrate deeply enough into the eye. If treatment becomes necessary, your physician will start with injections of steroid medication around the eye to suppress the immune system. These drugs are extremely helpful but, as with most therapies, side effects can and do occur. The most common side effects of injected steroids are cataracts and glaucoma.
On occasion, some patients have severe disease in both eyes and the best option is an oral agent that suppresses the immune system. Initially, steroid medications are used but most patients will need to be switched to a different medication such as cyclosporine A or methotrexate. Although these drugs can have serious side effects, most patients have no significant problems achieving a durable remission and retaining life-long high quality vision.
Schedule Pars Planitis Treatment in Northern California with Retinal Consultants Medical Group
Since 1975, Retinal Consultants Medical Group has been providing outstanding care to patients throughout Northern California, including Sacramento, Modesto, and Stockton. Our retina specialists and surgeons treat multiple vitreoretinal conditions, such as age-related macular degeneration and diabetic retinopathy. We invite you to contact us with any questions or schedule an appointment today.


