About Diabetic Retinopathy
What is diabetes and how can it affect my retina?
Diabetes refers to a group of diseases that affect your body’s ability to control blood sugar levels, causing them to rise higher and higher if not treated. Over time, high blood sugar can damage the small blood vessels in your eyes, kidneys, and other organs. The blood vessels in your retina are particularly sensitive to this injury. When diabetes causes damage to the retina and its blood vessels, we call this “diabetic retinopathy”.
Learn more about diabetic retinopathy at ASRS
Información en español en el sitio web de ASRS
What are the earliest signs that diabetic retinopathy is in my retina?
In the early stages of diabetic retinopathy, tiny capillary blood vessels become twisted and small spots of blood appear. We call this stage “nonproliferative diabetic retinopathy.” Monitoring your retina is important because the damage can progress to the more serious “proliferative diabetic retinopathy” that requires treatment to prevent blindness.
In addition to these forms of retinal damage, small capillary blood vessels injured from diabetes may leak fluid. In the normal retina, these capillaries are water-tight, like garden hoses, and they exchange oxygen and nutrients without oozing any blood or plasma. The fluid that leaks from diabetic blood vessels can build up in the retina, causing it to swell and blur your vision. We call this “diabetic macular edema.” Left untreated, diabetic macular edema can permanently damage the retinal nerve cells over time.
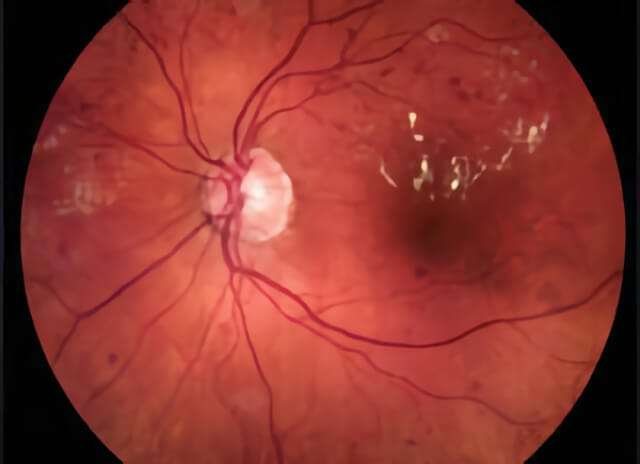
This color photograph illustrates areas of red dots and blots that indicate hemorrhage from diabetic damage to the retina. Also, there are white areas of fatty deposition in an area of swollen retina, a condition called diabetic macular edema.
How can diabetic macular edema be treated?
To stop the leakage and reduce the swelling caused by diabetes (diabetic macular edema), gentle laser treatment can be used to cauterize the leaky vessels. Injectable steroids or other medications may also be helpful, either alone or in conjunction with laser surgery. Commonly, these treatments are repeated over time because the problem typically recurs.
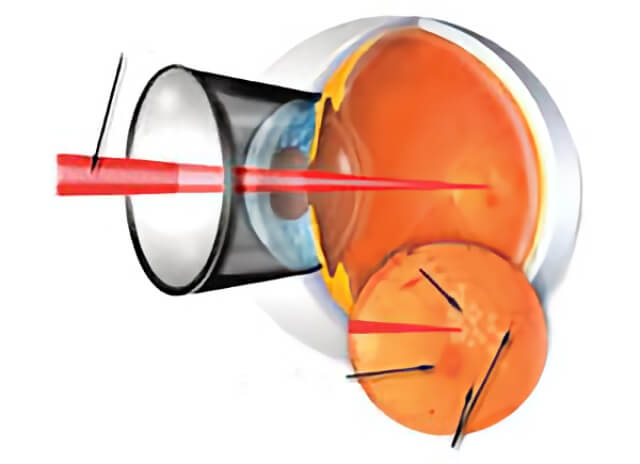
The laser treatment for diabetic macular edema is in an in-office procedure where small laser burns are carefully placed in the macula.
Therapy for diabetic retinopathy and macular edema is quite effective in preventing further vision loss, but only occasionally makes your vision better. Controlling your blood sugar with your primary medical provider is an important part of preventing further damage. As part of your eye evaluation, we may get a fluorescein angiogram or optical coherence tomography scan to help assess the level of damage and to guide treatment decisions.

A fluorescein angiogram demonstrating blocked and abnormal retinal blood vessels, as well as areas of neovascular vessels that are leaking (white, cloud-like areas).
Are there worse retina problems than diabetic macular edema and nonproliferative diabetic retinopathy that can occur from diabetes?
As diabetic retinopathy worsens, abnormal blood vessels start to grow on the retinal surface. We call this “proliferative diabetic retinopathy.” These new blood vessels are very fragile and can break, causing bleeding into the eye known as a “vitreous hemorrhage.” Even worse, this problem can cause your retina to detach, a potentially blinding problem requiring surgery.
In these cases, more aggressive laser treatment is applied to the retina to stop the vessel growth and prevent blindness. A common side effect is mild worsening of your night and reading vision, but in general this effect is minimal. In some cases of advanced diabetic retinopathy, normal blood vessels die off (called ischemia). The resulting nerve cell death from insufficient blood flow may permanently blur the vision.
What can be done for these more advanced forms of diabetic damage?
For more severe forms of diabetic retinopathy, injected medicines and lasers done in the office may be insufficient to prevent further loss of vision. In very advanced disease, an operation may be needed to clear out the blood in the eye or repair a retinal detachment. This operation, called vitrectomy, involves using miniature surgical instruments to restore a more normal space inside the eye and helps to optimize the function of the retina.
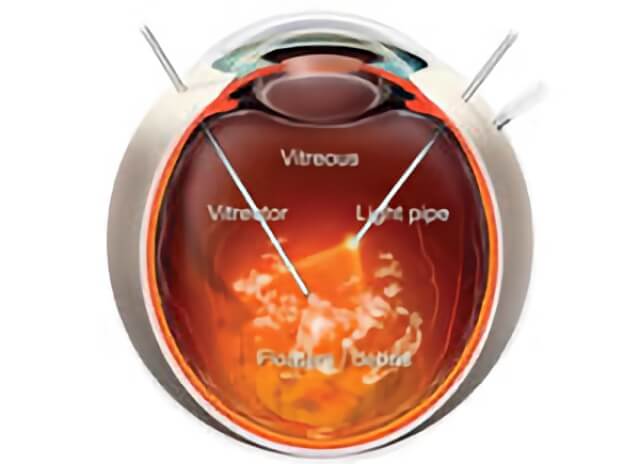
Sometimes, an operation called a vitrectomy is necessary to treat proliferative diabetic retinopathy. In this surgery, small incisions allow for microsurgical instruments to enter and operate in the vitreous cavity.
Schedule Diabetic Retinopathy Treatment in Northern California with Retinal Consultants Medical Group
Since 1975, Retinal Consultants Medical Group has been providing outstanding care to patients throughout Northern California, including Sacramento, Modesto, and Stockton. Our retina specialists and surgeons treat multiple vitreoretinal conditions, such as age-related macular degeneration and diabetic retinopathy. We invite you to contact us with any questions or schedule an appointment today.


